Sinus Pain/Pressure
Fullness, pressure or pain on the face – usually above the eyebrow, behind the eye and/or under the cheekbone.
Causes
- Viral Infection: Part of the common cold, infecting the lining of the nose and sinuses. Nasal washes with saline are recommended.
- Bacterial Infection: When the sinus becomes infected with bacteria, the main symptoms are increased sinus pain or return of fever. The skin around the eyelids or cheeks may become red or swollen. Thick nasal secretions that last over 14 days may point to an infection. Antibiotics by mouth are recommended.
- Allergic Reaction: Sinus congestion often occurs with nasal allergies (such as pollen). Sneezing, itchy nose and clear nasal discharge point to allergies.
Nasal Blockage/Obstruction
Partial or complete blockage of the breathing airway in the nasal cavity.
Causes
- Sinusitis (Acute or Chronic): Sinusitis is inflammation of the sinus cavities, often caused by allergies, colds, or nasal issues. Symptoms include headache, facial pain, congestion, and thick mucus. Treatments range from decongestants and antibiotics to surgery or balloon dilation for chronic cases.
- Nonallergic Rhinitis: Chronic congestion or sneezing not related to allergies.
- Nasal Polyps: Nasal polyps are benign growths in the nasal passages that can cause breathing issues. They’re common in adults with asthma or allergies and children with cystic fibrosis. Medications or surgery may be needed to treat them.
- Deviated Septum: Occurs when the thin wall (nasal septum) between your nasal passages is displaced to one side.
- Overuse of Decongestant Nasal Spray: Decongestant nasal sprays and drops should not be used for more than a week at a time. Longtime use can lead to increased obstruction.
- Allergies & Environmental Irritants: Occurs when the immune system reacts negatively to a foreign substance — such as pollen, bee venom, pet dander or specific foods. Nosebleeds Bleeding from 1 or both nostrils, not caused by an injury.
- Spontaneous: Most nosebleeds start up without a known cause.
- Rubbing/Blowing: Rubbing, blowing or picking at the nose is the most common cause.
- Sinus Infections: Main symptoms are dry snot and a blocked nose. This leads to extra nose blowing and picking. The sinus infection is more often viral than bacterial.
- Allergies & Allergy Medicines: Main symptom is an itchy nose, which leads to extra rubbing and blowing. While medicines help nasal symptoms, they also dry out the nose.
- Ibuprofen & Aspirin: These medicines increase bleeding tendency.
- Dry Air: Dryness of the nasal lining makes it more likely to bleed.
- Bleeding Disorder: This rare, but serious, condition means blood platelets or clotting factors are missing, or not working correctly. A bleeding disorder should be suspected if a nosebleed cannot be stopped, or excessive bleeding from the gums or from minor cuts occurs.
Endoscopic Sinus Surgery
Endoscopic sinus surgery (ESS) is a minimally invasive surgical procedure used to treat chronic sinus problems and other conditions affecting the sinuses. The surgery is performed using an endoscope, which is a small telescope with an attached camera, which allows the surgeon to view the inside of the nasal passages and sinuses on a monitor.
The primary goal of ESS is to clear blocked sinuses, remove obstructions like polyps or tumors, and improve drainage, which can help relieve symptoms such as chronic sinusitis, nasal congestion, and headaches. Unlike traditional open surgery, ESS is done through the nostrils, so there are no external incisions.
Common reasons for undergoing endoscopic sinus surgery include:
- Chronic sinusitis that hasn’t responded to medical treatment.
- Nasal polyps that cause obstruction.
- Structural issues in the nasal cavity, such as a deviated septum.
- Sinus tumors or other abnormal growths.
ESS typically has a quicker recovery time and less discomfort compared to traditional sinus surgery.
Turbinate Coblation & Reduction
Turbinate coblation, also called ablation, reduces the size of the turbinates (small curved bones in the nose) to improve breathing and alleviate symptoms like snoring, congestion, and sleep apnea. It’s a quick, minimally invasive procedure with little downtime, using either laser or radiofrequency energy to shrink the tissue.
Why Turbinate Reduction is Needed
Turbinate reduction is recommended when enlarged turbinates cause chronic nasal congestion, sinus infections, headaches, or sleep issues. If medications like decongestants and antihistamines don’t work, surgery may be needed.
Procedure and Recovery
Turbinate reduction is often done alongside septum correction (septectomy). It’s an outpatient procedure with minimal swelling and discomfort. Full recovery takes a few weeks, during which nasal sprays and follow-up visits help ensure proper healing. Once healed, patients experience significantly improved breathing and quality of life.
Reasons for Turbinate Reduction
Turbinate reduction is performed when a patient’s turbinate is abnormally large, creating a nasal obstruction. The turbinates may swell in response to ear, nose and throat allergies or upper respiratory infections, resulting in a number of troubling symptoms. These symptoms may include:
- Chronic nasal congestion
- Difficulty breathing through the nose
- Recurrent or chronic sinus infections
- Chronic nosebleeds
- Migraine headaches
- Snoring and sleep apnea
If traditional treatments, such as nasal decongestants, antihistamines, allergy shots and antibiotics do not resolve these problems, surgical intervention is usually recommended.
Balloon Sinuplasty
A balloon sinuplasty is a minimally invasive endoscopic procedure during which a thin balloon catheter is inserted into the nose. The balloon is gradually inflated to relieve blockages and widen the sinus pathways. The goal of a balloon sinuplasty is to enlarge the opening of the sinuses, reduce blockage and improve sinus drainage.
Under general anesthesia, a physician inserts a guide wire catheter equipped with a tiny balloon through the nostril in order to gain access to the blocked sinus passageway. The balloon is inflated, gently opening and widening the sinus passageway. It is then deflated and withdrawn, leaving an open sinus passageway that restores normal sinus drainage and function.
An endoscopic procedure performed under general anesthesia in an outpatient setting, balloon sinuplasty does not require incisions and cutting or the removal of bone and tissue. There is generally less pain, risk of infection, blood loss, bruising and swelling and many patients are often able to return to their normal activities in less time than they would from traditional “open” sinus surgery.
VivAer®
If you regularly experience difficulty breathing through your nose and nothing seems to help, you may have nasal obstruction. Until now, finding a long-term solution often meant surgery. Now, we may be able to offer you lasting relief without surgery (or incisions) by performing the VivAer® procedure to open your nasal airway.
Click here for more information!RhinAer®
If your nose is always runny, you may be one of the millions of people living with chronic rhinitis. For many patients, these symptoms may be caused by abnormal signals in the nose. The RhinAer® procedure is able to disrupt these signals and provide lasting relief without surgery (or incisions). The RhinAer® procedure is clinically demonstrated to improve symptoms in 96% of patients.1 Patients typically return to normal activity on the same day.
Click here for more information!Neuromark®
The NEUROMARK procedure is changing the game for chronic rhinitis sufferers, offering an effective treatment option. This in-office procedure treats chronic rhinitis at its source by using low-power energy to disrupt the overactive nasal nerves associated with chronic rhinitis.
Click here for more information!Hear how patients are breathing easier after their NEUROMARK procedure.
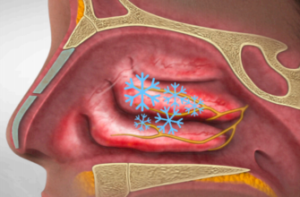
ClariFix® Cryotherapy for Chronic Rhinitis
ClariFix® cryotherapy is the first and only FDA cleared device for adults with chronic rhinitis, a condition characterized by frequent runny nose and congestion.

SINUVA™ Sinus Implant
SINUVA™ is a sinus implant that treats nasal polyps without surgery. During a routine office visit, Dr. Name will use topical and/or local anesthesia to numb the patient’s nose and sinuses. SINUVA™ is then placed in the sinus cavity through the nasal opening.

PROPEL®
PROPEL is a bioabsorbable stent placed following sinus surgery to keep the sinus open using a spring-like mechanism. The stent delivers steroid medication to the sinus tissue for up to 30 days. Over time, it dissolves on its own, so removal isn’t required, but the doctor can remove it at any time. PROPEL has been proven to reduce inflammation/edema and the need for oral steroids. In clinical studies, patients using PROPEL needed less post-surgery intervention at 30 days compared with patients not using PROPEL.
Septoplasty
Septoplasty is a surgical procedure to correct defects or deformities of the septum, the partition between the two nostrils. Commonly, the procedure is performed to correct a deviated septum. While a small deviation of the septum is commonplace, if the condition is severe, it may impede airflow through the nostrils. This may cause difficulty breathing and poor nasal drainage from the sinuses, both of which are problematic.
In adults, the nasal septum is composed of both cartilage and bone. The function of the nasal septum is to support the mucous membranes of the nose and to regulate air flow. Septoplasty is commonly performed to help relieve nasal obstruction and in some cases it may be a part of other surgical procedures including sinus surgery or nasal tumor or polyp removal. Septoplasty straightens the nasal septum by trimming, repositioning and replacing cartilage or bone within the nose.
In-Office Procedure Suite for minimally invasive nasal and sinus procedures
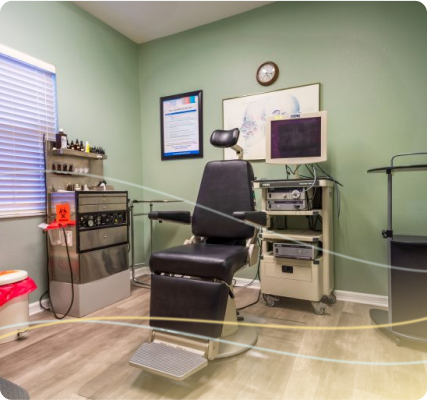
Florida E.N.T. & Allergy offers our patients a cutting edge technology in the comfort of the office. Using only topical/local anesthetic, we can treat your sinus disease. Our surgeons are trained and experienced to perform this procedure in the office. Florida E.N.T. & Allergy was the first practice in the West Florida region to perform these in the office and remains the leader in the area. This option offers a multitude of benefits from ease of recovery to immediate results. Here are some of the reasons this might be right for you.
- Local Anesthesia – we are able to avoid using general anesthesia and all the side effects that may come with it.
- Fast Recovery – by using the office setting with topical anesthesia, the recovery is almost immediate often without the need to stop medications that our patients may need to take. Often our patients also are able to avoid taking a full day off from work.
- Patient Satisfaction – With the quick recovery and high success rate we are able offer our patients the best of both worlds. This procedure allows us to avoid repeated antibiotic use and greatly reduce the need for further sinus surgery.
- Cost Saving – by avoiding hospital costs and avoiding missed work, some patients qualify for significant saving using this new technology in the office setting.


